Abstract
Introduction
Prostate cancer (PCa) is a heterogenous disease with multiple etiological factors playing a role in its development. Recently, chronic and systemic inflammatory conditions such as inflammatory bowel disease were identified as key risk factors influencing its development. The study aimed to evaluate the relationship between diverticular disease (DD) (local and acute inflammation) and PCa.
Methods
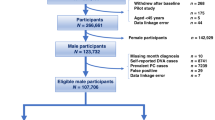
Hypertensive patients with DD and hypertensive controls were identified between 1995 and 2010 from the Statewide Planning and Research Cooperative System database. Cohorts were queried for PCa incidence through 2015. Univariable and multivariable logistic regression analyses were used for determining independent predictors of PCa diagnosis.
Results
A total of 51,353 patients with DD and 111,541 controls were identified. In all, 6.26% of DD developed PCa, and 3.71% of controls developed PCa (p < 0.01). DD was a significant risk factor for PCa (OR: 1.27 CI: 1.19–1.34, p < 0.01). On subgroup analysis, the patients diagnosed with DD <50 years old had an OR of 3.39 for PCa (CI: 2.52–4.56, p < 0.01), age 50–59 had an OR of 2.12 (CI: 1.86–2.15, p < 0.01), and age 60–69 had an OR of 1.20 (CI: 1.10–1.31, p < 0.01). Finally, age and race stratification showed that white patients <50 had an OR of 2.56 (CI: 1.75–3.76, p < 0.01), while black patients <50 had an OR of 3.98 (CI: 2.61–6.07, p < 0.01). The trend in differing odds between these populations was the same for age groups 50–59 and 60–69.
Conclusion
Our analysis shows that DD is associated with diagnosis of PCa in hypertensive men. Importantly, the earlier the diagnosis of DD, the higher the odds for development of PCa, particularly in black men.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Cancer Stat Facts: Prostate Cancer. National Cancer Institute. Surveillance, Epidemiology, and End Results Program. 2020. https://seer.cancer.gov/statfacts/html/prost.html
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2019. CA Cancer J Clin. 2019;69:7–34. https://doi.org/10.3322/caac.21551
Shoag J, Barbieri CE. Clinical variability and molecular heterogeneity in prostate cancer. Asian J Androl. 2016;18:543–8. https://doi.org/10.4103/1008-682X.178852
Gann PH. Risk factors for prostate cancer. Rev Urol. 2002;4 Suppl 5:S3–S10.
Shtivelman E, Beer TM, Evans CP. Molecular pathways and targets in prostate cancer. Oncotarget. 2014;5:7217–59. https://doi.org/10.18632/oncotarget.2406
Schoenborn JR, Nelson P, Fang M. Genomic profiling defines subtypes of prostate cancer with the potential for therapeutic stratification. Clin Cancer Res. 2013;19:4058–66. https://doi.org/10.1158/1078-0432.CCR-12-3606
Tomlins SA, Rhodes DR, Perner S, Dhanasekaran SM, Mehra R, Sun XW, et al. Recurrent fusion of TMPRSS2 and ETS transcription factor genes in prostate cancer. Science. 2005;310:644–8. https://doi.org/10.1126/science.1117679
Gonzalgo ML, Isaacs WB. Molecular pathways to prostate cancer. J Urol. 2003;170:2444–52. https://doi.org/10.1097/01.ju.0000085381.20139.b6
Grasso CS, Wu YM, Robinson DR, Cao X, Dhanasekaran SM, Khan AP, et al. The mutational landscape of lethal castration-resistant prostate cancer. Nature. 2012;487:239–43. https://doi.org/10.1038/nature11125
Prostate Cancer Risk Factors. American Cancer Society. 2020. https://www.cancer.org/cancer/prostate-cancer/causes-risks-prevention/risk-factors.html
Giovannucci E, Liu Y, Platz EA, Stampfer MJ, Willett WC. Risk factors for prostate cancer incidence and progression in the health professionals follow-up study. Int J Cancer. 2007;121:1571–8. https://doi.org/10.1002/ijc.22788
Burns JA, Weiner AB, Catalona WJ, Li EV, Schaeffer EM, Hanauer SB, et al. Inflammatory bowel disease and the risk of prostate cancer. Eur Urol. 2019;75:846–52. https://doi.org/10.1016/j.eururo.2018.11.039
Ge YQ, Shi QQ, Yao WX, Cheng Y, Ma GX. The association between inflammatory bowel disease and prostate cancer risk: a meta-analysis. Prostate Cancer P D. 2020;23:53–58. https://doi.org/10.1038/s41391-019-0177-7
Violi A, Cambie G, Miraglia C, Barchi A, Nouvenne A, Capasso M, et al. Epidemiology and risk factors for diverticular disease. Acta Biomed. 2018;89:107–12. https://doi.org/10.23750/abm.v89i9-S.7924
Omidele OO, Davoudzadeh N, Palese M. Fellowship and subspecialization in urology: an analysis of robotic-assisted partial nephrectomy. Urology. 2019;130:36–42. https://doi.org/10.1016/j.urology.2019.03.028
Omidele OO, Davoudzadeh N, Shah M, Tomer N, Palese M. Trends in utilization and perioperative outcomes in live donor nephrectomies: a multi-surgical discipline analysis. World J Urol. 2019;37:2225–30. https://doi.org/10.1007/s00345-018-2559-1
Ravivarapu KT, Omidele O, Pfail J, Tomer N, Small AC, Palese MA. Robotic-assisted simple prostatectomy versus open simple prostatectomy: a New York statewide analysis of early adoption and outcomes between 2009 and 2017. J Robot Surg. 2020. https://doi.org/10.1007/s11701-020-01152-w
Fryar, C. D., Ostchega, Y., Hales, C. M., Zhang, G. & Kruszon-Moran, D. Hypertension Prevalence and Control Among Adults: United States, 2015–2016. NCHS Data Brief, 1–8 (2017).
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40:373–83. https://doi.org/10.1016/0021-9681(87)90171-8
Nettey OS, Walker AJ, Keeter MK, Singal A, Nugooru A, Martin IK, et al. Self-reported Black race predicts significant prostate cancer independent of clinical setting and clinical and socioeconomic risk factors. Urol Oncol. 2018;36:501 e501–501 e508. https://doi.org/10.1016/j.urolonc.2018.06.011
Coussens LM, Werb Z. Inflammation and cancer. Nature. 2002;420:860–7. https://doi.org/10.1038/nature01322
Korniluk A, Koper O, Kemona H, Dymicka-Piekarska V. From inflammation to cancer. Ir J Med Sci. 2017;186:57–62. https://doi.org/10.1007/s11845-016-1464-0
Grivennikov SI, Greten FR, Karin M. Immunity, inflammation, and cancer. Cell. 2010;140:883–99. https://doi.org/10.1016/j.cell.2010.01.025
Greten FR, Grivennikov SI. Inflammation and cancer: triggers, mechanisms, and consequences. Immunity. 2019;51:27–41. https://doi.org/10.1016/j.immuni.2019.06.025
Jiang J, Li J, Yunxia Z, Zhu H, Liu J, Pumill C. The role of prostatitis in prostate cancer: meta-analysis. PLoS One. 2013;8:e85179 https://doi.org/10.1371/journal.pone.0085179
Sfanos KS, Yegnasubramanian S, Nelson WG, De Marzo AM. The inflammatory microenvironment and microbiome in prostate cancer development. Nat Rev Urol. 2018;15:11–24. https://doi.org/10.1038/nrurol.2017.167
Barroso AO, Quigley EM. Diverticula and diverticulitis: time for a reappraisal. Gastroenterol Hepatol (N Y). 2015;11:680–8.
Feuerstein JD, Falchuk KR. Diverticulosis and diverticulitis. Mayo Clin Proc. 2016;91:1094–104. https://doi.org/10.1016/j.mayocp.2016.03.012
Freeman HJ. Segmental colitis associated diverticulosis syndrome. World J Gastroenterol. 2016;22:8067–9. https://doi.org/10.3748/wjg.v22.i36.8067
Schembri J, Bonello J, Christodoulou DK, Katsanos KH, Ellul P. Segmental colitis associated with diverticulosis: is it the coexistence of colonic diverticulosis and inflammatory bowel disease? Ann Gastroenterol. 2017;30:257–61. https://doi.org/10.20524/aog.2017.0126
Carter H, Albertsen P, Barry M, et al. Early Detection of Prostate Cancer. AUA Guidelines. 2018. https://www.auanet.org/guidelines/guidelines/prostate-cancer-early-detection-guideline
Rezapour M, Ali S, Stollman N. Diverticular disease: an update on pathogenesis and management. Gut Liver. 2018;12:125–32. https://doi.org/10.5009/gnl16552
Carlson DS, Grivas P, Wei W, Dhillon PK, Abraksia S. The effectiveness of shared compared to informed decision making for prostate cancer screening in a high-risk African American population: a randomized control trial. Cancer Invest. 2021;39:124–32. https://doi.org/10.1080/07357907.2020.1855441.
Merrill RM, Lyon JL. Explaining the difference in prostate cancer mortality rates between white and black men in the United States. Urology. 2000;55:730–5. https://doi.org/10.1016/s0090-4295(99)00564-6
Dess RT, Hartman HE, Mahal BA, Soni PD, Jackson WC, Cooperberg MR, et al. Association of black race with prostate cancer-specific and other-cause mortality. JAMA Oncol. 2019;5:975–83. https://doi.org/10.1001/jamaoncol.2019.0826
Dovey ZS, Nair SS, Chakravarty D, Tewari AK. Racial disparity in prostate cancer in the African American population with actionable ideas and novel immunotherapies. Cancer Rep (Hoboken). 2021;e1341. https://doi.org/10.1002/cnr2.1340.
Rayford W, Beksac AT, Alger J, Alshalalfa M, Ahmed M, Khan I, et al. Comparative analysis of 1152 African-American and European-American men with prostate cancer identifies distinct genomic and immunological differences. Commun Biol. 2021;4:670 https://doi.org/10.1038/s42003-021-02140-y
Yeo LX, Tseng TH, Chen WL, Kao TW, Wu LW, Fang WH, et al. Hypertension control and risk of colonic diverticulosis. Ther Adv Gastroenterol. 2019;12:1756284819855734 https://doi.org/10.1177/1756284819855734
Gill D, Georgakis MK, Koskeridis F, Jiang L, Feng Q, Wei WQ, et al. Use of genetic variants related to antihypertensive drugs to inform on efficacy and side effects. Circulation. 2019;140:270–9. https://doi.org/10.1161/CIRCULATIONAHA.118.038814
Author information
Authors and Affiliations
Contributions
Conceptualization: NT, DC, and AKT; data collection, methodology, and formal analysis: NT and PR; writing (original draft preparation): NT and DC; writing (review and editing): NT, DC, PR, NM, IJ, ZD, MAP, and AKT; tables and figures: NT, IJ, and PR. All authors have provided critical feedback and have approved the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Tomer, N., Chakravarty, D., Ratnani, P. et al. Impact of diverticular disease on prostate cancer risk among hypertensive men. Prostate Cancer Prostatic Dis 25, 700–706 (2022). https://doi.org/10.1038/s41391-021-00454-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-021-00454-w